Why
Choose Homebirth?
Giving
birth naturally can be an experience of transformation and empowerment
for everyone involved, and yet the intensity of the process can
be challenging for many women. The key to a birth that is both
healthy and minimally painful is the ability to relax, as it allows
the spontaneous rhythms of labor to progress without interference.
The greatest obstacle is fear, for it generates tension and resistance
and makes coping with contractions more difficult. In general,
the more relaxed the mother, the easier the birth.
Mothers birth best where they feel the most comfortable. For many
healthy, low-risk mothers, home provides a supportive and safe
environment in which to give birth. Moreover, when a newborn baby
is perceived to be a conscious, cognizant being, the manner in
which he/she is born can have far reaching effects both psychologically
and spiritually. In the privacy and sanctity of home, a mother
can surround herself with those she loves and trusts. Assisted
by capable, experienced practitioners, the family has more freedom
to create the experience they desire and welcome their new child
with love and dignity.

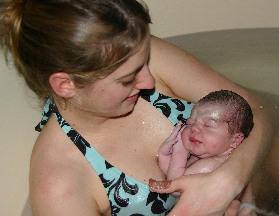
Emily
reaches for her son as he emerges from her body.
There is no more amazing moment........
"Where
would all the specialists and producers of medical technology
and drugs be if it were suddenly 'discovered' that when
women eat well in pregnancy, eliminate drugs and stop
substance abuse, almost all complications disappear?" -
Anne Frye
Advantages
for Mother
-
Childbirth has the potential to be a profound, life-transforming
experience for the woman, one which may facilitate emotional
healing, strengthen and deepen her relationships to all aspects
of herself--with far reaching effects to her children, her mate
and family members.
-
She is not subjected to routine procedures such as continuous
electronic fetal monitoring, IVs, and episiotomy.
-
She can eat, drink, walk, and rest freely, working with her
own natural body rhythms.
-
She has continuous care with the same attendant throughout
the prenatal, labor, delivery and postpartum periods, facilitating
trust and competent decision-making based on process as an individual.
-
She
is more likely to deliver without drugs, vacuum extractors or
cesarean section when supported by caregivers who feel that
birth is a normal physiological function.
-
The woman and baby have less risk of infection in her own home.
-
She
is free to explore a variety of creative birthing options such
as waterbirth, birthing stools, delivery positions like squatting
or hands and knees, and may utilize comfort measures like candles,
incense, inspiring music, and aromatherapy.
-
She
is less likely to experience postpartum depression when she
has not been separated from her baby. In addition, when childbirth
takes place at home, it becomes an integral part of family life,
with father and/or siblings able to participate in as complete
and appropriate a manner as possible. This assists postpartum
adjustment for all family members.

Joelle
sitting with her daughter Courtney during her labor. Joelle was
very relaxed during her labor. She was about 7 cms dilated at the
time of this picture.
-
The
baby's experience at birth can be made as gentle and loving
as possible, and routine procedures such as deep suctioning,
bright lights and artificial warming can be avoided unless medically
necessary.
-
The
healthy baby remains with the mother, preserving the mother-infant
bonding so crucial to the development of attachment parenting.
-
The
baby is more likely to be born vaginally without breathing difficulties
so often associated with anesthetics and cesarean birth.
-
Breastfeeding
is easier to establish when the baby can nurse on demand, and
the mother is given immediate encouragement and instruction
in proper technique.
-
Baby
is less likely to develop an infection at home.

Joelle
& new baby Callie, surrounded by older sisters Chloe and Courtney,
and proud daddy Tim, relaxing together in bed after the birth.
-
Requires a higher level of effort and responsibility on the
part of the parents, and may not be supported by medical doctors/society.
While midwives are trained in emergency measures, access to
some equipment may be delayed, and transport to a hospital may
be required. In urban areas, access to emergency medical services
are expeditiously obtainable, and most midwives work in consultation
and collaboration with an obstetrician who is willing to assume
care of their patients if necessary.
________________________________________________
SAFETY
OF HOMEBIRTH
There
have been a number of clinical studies on the safety of homebirth
for normal, low-risk women receiving good prenatal care. Practically
all of them show that homebirth is either as safe, or safer, than
hospital birth - for low risk, healthy pregnant women with normal
pregnancies. The main study describing homebirth as more dangerous
is a study that was done by the American College of Obstetricians
and Gynecologists in 1978 called "Health Department Data Shows
Danger of Homebirths." This study included all out-of-hospital
births, including unattended births in the home, births en route
to the hospital, mothers who may have been high risk, had received
no prenatal care, and babies who were pre-term. This factor, which
skewed the results, was not widely acknowledged. In fact, this
report also included miscarriages in its data showing the risks
of homebirth. Clearly, this report is not representative of the
kind of homebirth that midwives are offering. And interestingly
enough, it seems to be the ONLY study that showed homebirth to
be less safe than hospital birth, although many studies have tried.
To
read more about the safely of homebirth with skilled midwives, read The Five Standards for Safe Childbearing, by David
Stewart, Ph.D. It cites study after study that detail the statistics
that prove the safety of midwife-attended homebirth.
_
Kristin and newborn Grant, 12/15/2002: the
euphoria of giving birth naturally.
___________________________________________
The
Philosophical Assumptions of Home Birth Parents and Attendants*
-
Because
pregnancy and birth are natural physiological events, normal
birth does not belong in hospitals.
-
The
natural course of labor is already perfect, and should be interfered
with as little as possible. Pain is part of an essential and
healthy feedback mechanism in labor, which women can learn to
cope with, with proper encouragement and support.
-
Medical
management of pregnancy and birth should be limited to those
that are medically complicated.
-
Unnecessary
medical interventions complicate normal labor, creating additional
risk and the need for more intervention.
*excerpt taken from Birthing from Within by Pam
England, CNM, MA, and Rob Horowitz, Ph.D.
______________________________________________________
"There
is, in fact no scientific support for the vast majority of
interventions
that are commonly used in maternity care today."
Doris
Haire, President, American Foundation for Maternal and Child
Health

Baby
Noah, about an hour after he was born.
Home
Birth and Out-of-Hospital Birth: Is it Safe?
How Safe is that Hospital Anyway?
Information compiled by Jennifer L. Griebenow
4/97
In
the past, most Americans were born at home with lay midwives attending.
The mortality rate for both mothers and babies was higher in 1900,
at 700 maternal deaths per 100,000 births, than it is now. Babies
also died at a significantly higher rate at that time, which decreased
to 28.9 births per thousand by 1960. Obstetricians tend to emphasize
that many women used to die in childbirth, implying that we should
be grateful for current obstetric practice. However, even in 1900,
the percent of women who died giving birth was only 7/10ths of one
percent! One has to wonder how this percentage compares with our
country's current cesarean section rate of 22%.
Are
the surgeries performed on these mothers actually saving them from
imminent death? Maternal and infant mortality are lower now than
they were 40 years ago. But the assumption that hospital birth is
safer for mother and baby has never been supported. Prenatal care,
better nutrition, antibiotics and blood transfusion have played
more of a part in the relative safety of birth now. Sheila Kitzinger,
British childbirth expert, states that planned home birth with an
experienced lay midwife has a perinatal death rate of 3-4 babies
per 1,000 births. Hospital births, by contrast, carry a perinatal
mortality rate of 9-10/1,000. [Perinatal death rates include fetal
deaths on and after 28 weeks gestation, whereas neonatal mortality
rates only include deaths occurring in the first 28 days after.)A
study in Australia found a perinatal mortality rate of 5.9/1,000
out of 3400 planned home births.
-
Joseph C. Pearce states in his landmark book Evolution's End that
homebirthed babies have a six to one better chance of survival
than a hospital-birthed child.
- A
study in the Netherlands done in 1986 on women who were having
their first babies showed these results: out of 41,861 women who
delivered in the hospital, the perinatal mortality rate was 20.2/1,000.
Of 15,031 women who delivered at home with a trained midwife,
the rate was 1.5/1,000 . I know, I thought it must be a typo too.
- Marsden
Wagner, formerly of the World Health Organization, states that
every country in the European Region that has infant mortality
rates better than the US uses midwives as the principal and only
attendant for at least 70% of the births. He also states that
the countries with the lowest perinatal mortality rates in the
world have cesarean section rates below 10%. How does this compare
with the US rate? Miserably.
Cesarean
section and hospital birth is not doing for women and their newborns
what doctors and hospitals claim it is! Ask for statistics and studies
when your doctor claims hospital birth is safer than planned (not
accidental, unattended) home birth. He will be unable to provide
them. If your doctor says, "That's common knowledge," you would
be wise to seek another health care provider. If you can find studies
that claim hospital birth is safer, you will find that they included
deaths occurring in unplanned, unattended births that occurred at
home, rather than comparing normal, low-risk women. And more often
than not, the study will have been funded by (guess who?) ACOG (The
American College of Obstetricians & Gynecologists). Other studies:
- Lewis
Mehl did a study comparing home and hospital birth with mothers
from California and Wisconsin with matched populations of 2,092
mothers for each group. Midwives and family doctors attended the
homebirths; OB-GYNs and family doctors attended hospital births.
Within the hospital group, the fetal distress rate was 6 times
higher. Maternal hemorrhage was 3 times higher. Limp, unresponsive
newborns arrived 3 times more often. Neonatal infections were
4 times as common. There were 30 permanent birth injuries caused
by doctors.
- Dr.
Mehl did another study comparing 1,046 home births with 1,046
hospital births. The groups were matched for age, risk factors,
etc. There was no difference in infant mortality. None! However
the hospital births caused more fetal distress, lacerations to
the mother, neonatal infections and so on. There was a higher
rate of forceps and C-section delivery and nine times as many
episiotomies.
- o
Robert C. Goodlin reported in the Lancet on 1,000 births, half
occurring in a hospital, half in a birth center. There were no
IVs, monitors or anesthesia used in the birth center, but the
babies were born in better condition. Besides that, three times
as many cesareans were performed in the hospital.
- In
1982, Anita Bennett and Ruth Lubic evaluated 2000 births that
had happened in 11 freestanding birth centers. The neonatal death
rate was 4.6/1,000. The authors were denied information on low-risk
women delivering in hospitals. One wonders why....
- A
British research statistician, Marjorie Tew, did long term studies
of the safety of birth in various settings during the 1980s. She
found that among a sample of 16,200 births, the perinatal mortality
rate was lower for out-of-hospital births, even for very high-risk
mothers! At a relatively high-risk level, perinatal mortality
was three times higher in hospital. Tew then expanded her research
by using information from the Netherlands, a nation where both
obstetricians and midwives practice. The perinatal mortality rate
was ten times higher in the hospital births there, even though
the risk status of the mothers at the time of delivery was not
much higher than that of mothers who chose midwives.
- In
the Netherlands, which has a significantly lower infant mortality
rate than ours, the C-section rate is 7%. The episiotomy rate
is 6%, whereas ours is as high as 90%. Midwives attend most of
the births in the Netherlands. (Midwives tend to allow time for
the woman's tissues to stretch and to use perineal massage, warm
compresses, and good head flexion to avoid both episiotomies and
tearing; hence the lower Netherlands rate.)
- In
1988, the US ranked 19th among industrialized nations for low
infant mortality rates. By comparison, Sweden, where all mothers
receive midwifery care, even when they are high risk and may also
require physician care, ranked second.
- Between
1978 and 1985, licensed midwives in Arizona had a perinatal mortality
rate of 2.2/1,000 and a neonatal mortality rate of 1.1/1,000.
o In Madera County Hospital in California, where there is a transient,
high-risk population, midwives did the best job. In 1959, when
doctors did the deliveries the neonatal mortality rate was 23.9/1,000.
During 1960-1963, midwives had a rate of 10.3/1,000. When OBGYNs
took over again in 1964, the rate skyrocketed to 32.1/1,000.
Carl
Jones says, and I concur, "No one can tell a mother she is perfectly
safe giving birth at home. Whether she is safer at home than in
a hospital, however, is another question". There is always going
to be some risk when giving birth, as in all of life, and women
should be carefully screened for any health problems that could
be dangerous during labor and delivery. For certain women in rare
instances, obstetric care is essential. However, for most women,
better, healthier results are seen when mothers choose birth centers
or home births. As far as the risk of home birth goes, Our Bodies,
Ourselves states, "The times when hospital care unexpectedly becomes
instantaneously necessary are rare".

Nikki
was in active labor when her husband Fred joined her in the labor
tub.
She stayed there until her baby was born
In
A Good Birth, A Safe Birth, Diana Korte and Roberta Scaer
quote Tew, the research statistician, who says, "The danger of home
as a place of birth does not lie in its threat to the healthy survival
of mothers and babies, but in its threat to the healthy survival
of obstetricians and obstetric practice".
Another
factor that is important in making the choice about where to give
birth may surprise you. It makes common sense, but has also been
documented by several studies. Women who give birth in a hospital
are much more likely to experience postpartum depression or even
post traumatic stress disorder. Kitzinger states that the more interventions
a woman experiences, the more likely she is to be depressed, with
C-sections obviously carrying the greatest risk of depression. She
quotes 5 or 6 studies documenting the effects of this "institutional
violence." Aidan McFarlane, a British physician, notes that while
68% of hospital mothers experience postpartum depression, only 16%
of home birth mothers do. On The Farm, a self-contained, alternative
lifestyle community in Tennessee, the rate of postpartum depression
was .03 percent. Almost all mothers on the Farm had both a homebirth
and a supportive, loving community of women to assist them postpartum.
Avoiding depression, in itself, would be a major reason for mothers
to consider giving birth in their own homes, if that is where they
are most comfortable, especially if they had previously experienced
postpartum depression and thus were at high risk for a repeat episode.
Aspects
of hospital birth that may strongly contribute to the incidence
of postpartum depression in our country are the way the moment of
birth is handled and the routine separation of baby and mother.
In a study that appeared in the New England Journal of Medicine
in 1972, Marshall Klaus, the "bonding" expert, found that holding
the baby close released "dormant intelligences" in the mother and
caused "precise shifts of brain functioning and permanent behavior
changes". In other words, bonding is not just an emotional thing
that only mothers think happens. It is a biochemical process that
forever changes the mother, so that she knows more instinctively
how to relate to her baby. In the hospital, baby cannot see mom
with all the bright lights and is often inspected and observed for
several hours before mother can hold it for any length of time.
This is not to say love can't make up for this loss, but motherhood
might come easier if we had those natural body changes to help us.
Then
babies are still routinely kept in the nursery, if not most of the
time, at least part of the time. The routine separation of mom and
infant makes baby frightened and mom depressed. This may be why
postpartum depression and difficult adjustments are so common in
the US and rare elsewhere. Japan moved from midwifery to obstetrical
handling of births approximately 25 years ago. When older Japanese
recently asked Joseph Pearce why their mothers no longer "know what
to do with their children," one has to wonder how much the new hospital
setting has to do with it.
Most
homebirth studies also show a significantly lower rate of C-section
than hospitals have. Most stats show a rate between 1-5% for planned
homebirths, with the above-quoted lower mortality rates as well.
Cesarean sections themselves carry a far greater risk of additional
illness or death than most people realize. They have become so routine
in our society that everyone feels "It's no big deal." However,
C-sections carry a 2 to 4 times greater risk of death than do vaginal
deliveries (Boston Women's Health Book Collective). Several studies
on the risk of death from the surgery alone (i.e. factoring out
the conditions the surgery was done for) have shown varying, yet
consistently depressing, results. Errard and Gold found with eleven
years of statistics that the risk of death from cesarean section
was 26 times greater than from vaginal birth. Cohen and Estner also
cite a study done in Georgia showing a maternal death rate of 59.3
per 100,000 women who had cesarean section versus 9.7/100.000 for
women who delivered vaginally. A California study showed a maternal
death rate 2-3 times greater from C-section. Korte and Scaer state
that obstetricians admit a maternal death rate four to six times
higher with cesareans, and add that many believe the rate is higher,
giving 1 in 1,000 as the true odds of death for a c-section mother.
Lindsay
gave birth to her first baby, Valen, in the Jacuzzi tub in their
home just moments before this photo. Her labor was 3.5 hours total!
You
should also be aware that death is not the only complication caused
by cesareans; mothers commonly experience infection after a section.
Infertility problems, organ damage, and paralysis from anesthesia
complications are rare but possible risks. The pain at the incision
site is no picnic either. Another thing to think about is how a
surgery like this will affect you, your child, and your society
in the long run. When mothers "fail" to give birth naturally in
hospitals, as they so often do these days, their self image is harmed
despite well meaning friends telling them it doesn't matter how
baby came out. Especially if mothers are not certain their sections
were absolutely necessary, there is often a hidden anger that can't
be overtly expressed in our culture. Mothers may take this unacceptable
anger out on the only people they can--their children. "In 1979,
the government of California funded the first scientific study ever
made of the root causes of crime and violence. Their first report
three years later stated that the first and foremost cause of the
epidemic increase of violence in America was the violence done to
infants and mothers at birth".
The
"little things" really do matter, just as a small pebble thrown
in a pond makes ripples that travel a long, long way. If you are
a woman with no health problems or contraindications to safe labor
and delivery, consider very carefully your place of birth. Your
chance of having major surgery is one in four if you choose a hospital,
regardless of your current health status. Those are very good odds.
If you had the opportunity to buy a million dollar lottery ticket
with odds that good, you would, wouldn't you? Don't assume that
it won't happen to you. Since the risks to you and your baby are
lower at home, and your risks of having surgery are greater if you
go to a hospital, please consider homebirth as an option.
Wherever
you decide to give birth is up to you; just remember that you can
make the decisions that need to be made when you have true information.
It is your body, your baby, your money, and your life on the line,
not the doctor's or anyone else's. You have the right to accurate
information and the right to decide what is best for your baby.
Don't let anyone tell you otherwise. Also, when you ask for information,
beware of health care providers who say they judge each case individually,
so they can't really give you their statistics. It probably means
either they don't know or they don't want you to know. You will
have to live with the consequences of decisions made during your
labor, for better or worse. For more information or support, call
me at 606/625-0185 or email me at griebenow@iclub.org
The
author disclaims any liability resulting from the use of this information,
and strongly urges you to use your own mind.

Lindsay
and Steve fall in love with their baby.
_________________________________________________________
|
















